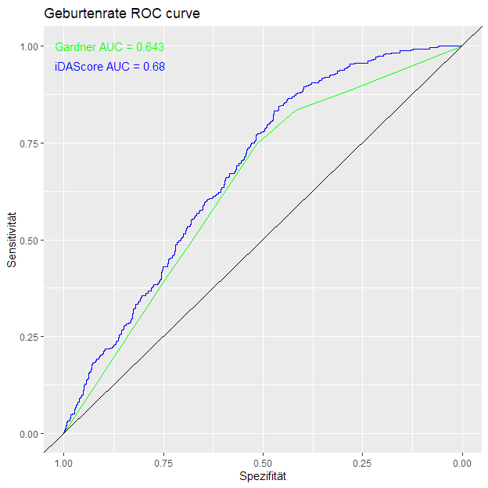
In the Embryoscope, the division behaviour of the embryo is continuously recorded using time-lapse photography under stable culture conditions. The various morphological changes are evaluated using a neural network (iDAScore). After examining a large number of embryos, this accumulated data was then correlated with clinical parameters such as the birth rate after implantation of a single embryo. Compared to the subjective morphological assessment by biologists (Gardner score), this score, which is determined objectively using artificial intelligence (AI), is generally more reliable in terms of prognosis and therefore also has a higher predictive value (ROC-AUC 0.68 vs. 0.64; see graph), see also the publication from our centre attached below.